“Little Fires Everywhere.
That’s how I describe the climate of cultural competence in healthcare for, quite frankly, the history of modern medicine as we know it. From the non-English speaking family that feels uncomfortable asking a follow up question after their provider has disconnected with interpreter services to the woman who practices Islam only being offered male providers, countless patients in America risk unfavorable outcomes solely because cultural competence and representation in healthcare are not prioritized as highly as they should be. These “little fires rarely make the evening news, nor are they even discussed in morbidity and mortality conferences- the fires are “put out in the moment and disregarded afterward. But how did that experience impact the patient’s trust in healthcare? Has that experience changed how the patient will interact with healthcare in the future for the worse?
The Moment that Ignited Little Fires
There was a moment in my first pediatric nurse practitioner position that opened my eyes to just how many little fires erupt in healthcare everyday. It was the first week of school (pre-COVID-19) and a teenaged young lady was struggling with a very dry, flaky & itchy scalp for weeks. When I walked into the exam room, I complimented her beautiful braided hairstyle and reminisced with her mom on how excited we were to show off our new hairstyles at school on the first day. My patient reminded me it took over 4 hours to get her hair braided and how much she loved the style- it felt great knowing I could relate to my patient in this way.
After looking over her scalp and reviewing her medical history, I determined my patient’s concern would be best treated by a medicated shampoo, however, my patient JUST got her beautiful braids done, how could I ask her to remove them?!
I reached out to my more experienced colleague for alternative options- he, an older Asian man, told my patient and her mom that they’d just have to “suck it up and remove the braids for this treatment. The looks on their faces made it clear the plan wouldn’t work for them.
I wasn’t satisfied.
The Search for a Seborrheic Dermatitis Treatment for Black Hair
I spent the next 15 minutes conducting an extensive literature review for the treatment of seborrheic dermatitis, my patient’s diagnosis.
Seborrheic dermatitis is a skin condition affecting a person’s scalp. It is often observed as scaly patches, red skin, and recurring dandruff. This skin condition can affect both oil and dry areas of the body. Seborrheic can disappear without treatment, but may also require multiple treatment sessions before completely going away. – MayoClinic
I found that while the gold standard treatment is a medicated shampoo, medicated topical oils can be used in lieu of a shampoo. I discussed the options with mom and we decided the oil would be a great option until she removes the braids and could use the shampoo.
Two months later, she returned to my office with a flake-free scalp and a hug, thanking me for looking into the alternative option.
The Importance of Diversity & Representation in Healthcare
I often think about how the situation would’ve played out if I wasn’t her provider- if she didn’t have a provider who wholeheartedly understood her perspective. Of course a hair style isn’t more important than health, but if an alternative exists that can satisfy the patient’s lifestyle (whatever it may be) and their medical needs, why not offer it? My colleague wasn’t even willing to listen to the reason the shampoo wasn’t the best option for my patient- how many times does this happen to patients each day?
Throughout my time in that office, there were dozens of little fires that had been burning for years that I officially put out- from converting from the brand name to generic for affordability to calling specialty provider offices to find extended hours for a working single parent. How many times have patients agreed to a plan they were uncomfortable with or unable to do solely because they didn’t feel seen by their providers?
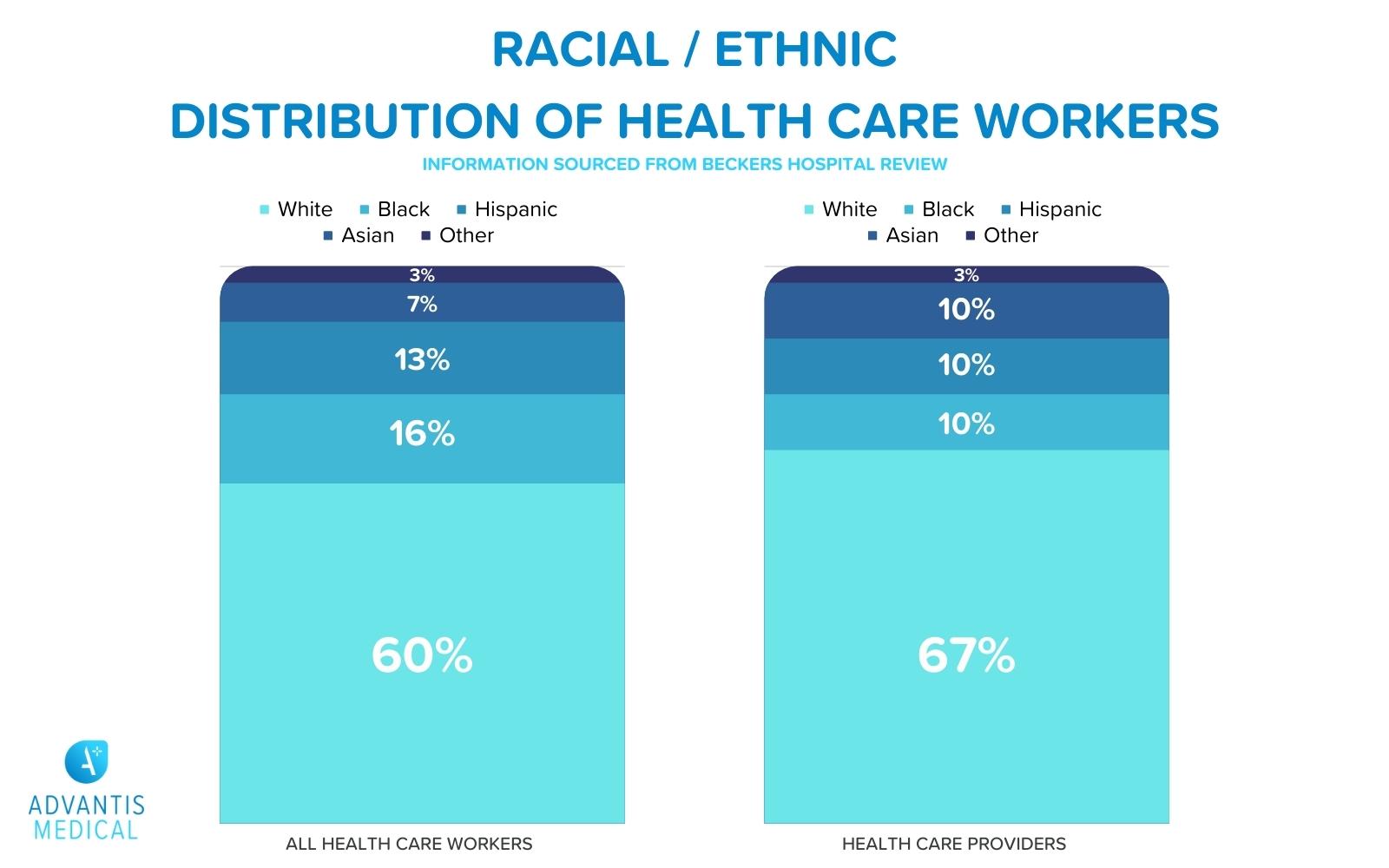
Representation matters in every professional setting but a lack of representation can lead to serious negative outcomes in healthcare. Which little fire will it take to spark change?









