Throughout the COVID-19 pandemic, many nurses have reported symptoms of Post-Traumatic Stress Disorder (PTSD). With no end in sight for many months, many nurses feared another PPE shortage, spreading the virus to their loved ones, or more deaths due to Covid. However, PTSD in nurses has existed within the nursing profession long before the COVID-19 pandemic.
History of PTSD
As with many mental health conditions, PTSD has not been adequately recognized or treated throughout much of human history. For hundreds of years in the U.S., this mental health disorder was only recognized among men with traumatic war experiences.
Only 51 years ago, in 1970, was PTSD recognized as a valid mental health diagnosis for all individuals. And even though it became diagnosable, receiving proper treatment remained nearly impossible.
Even today, many nurses experiencing mental illnesses such as PTSD due to their work do not feel that they are receiving the proper support from their workplace. Most do not feel seen or heard but instead silenced.
PTSD in Nurses
There are many potential symptoms of PTSD that a nurse might develop following a traumatic event. The following are some of the possible symptoms of PTSD in nurses:
- Insomnia
- Nightmares
- Irritability
- Hyper-vigilance of stable patients
- Easily angered
- Feelings of detachment
- Easily startled
- Exaggerated negative beliefs, taking fault for patients’ traumatic situations.
- Inability to concentrate
- Avoiding rooms where traumatic experiences occurred
- Fatigue
Every nurse is different, and not every nurse will have the same response to a traumatic situation. Studies have shown that nurses with a background of trauma and abuse, or nurses who have experienced multiple traumatic problems on the job, are more at risk for developing PTSD.
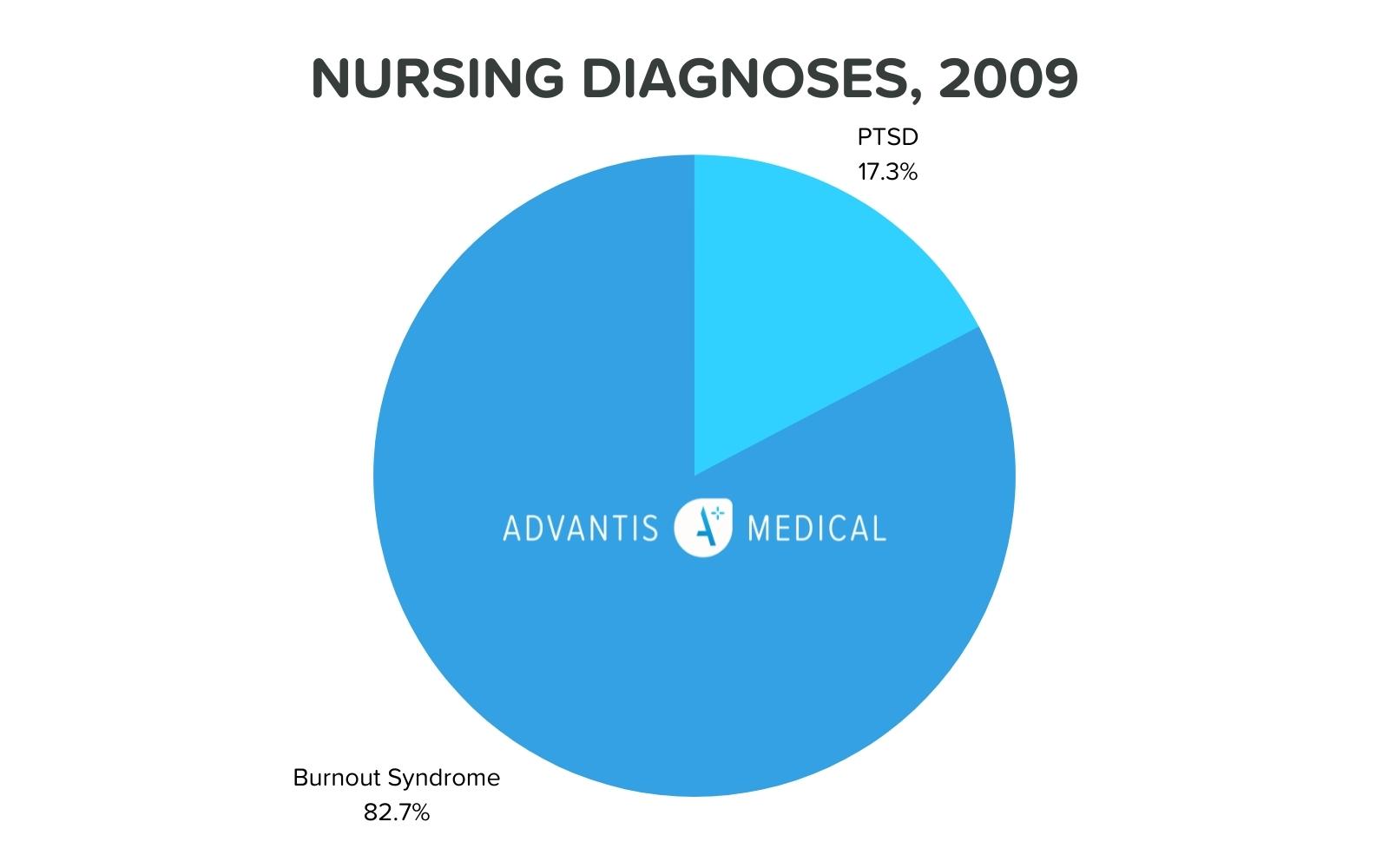
A 2009 study published by the Department of Health and Human Services and the National Institutes of Health found that out of the 41% of nurses who responded to the questionnaire, 18% met the criteria for a PTSD diagnosis, and 86% met the criteria for Burnout Syndrome (BOS).
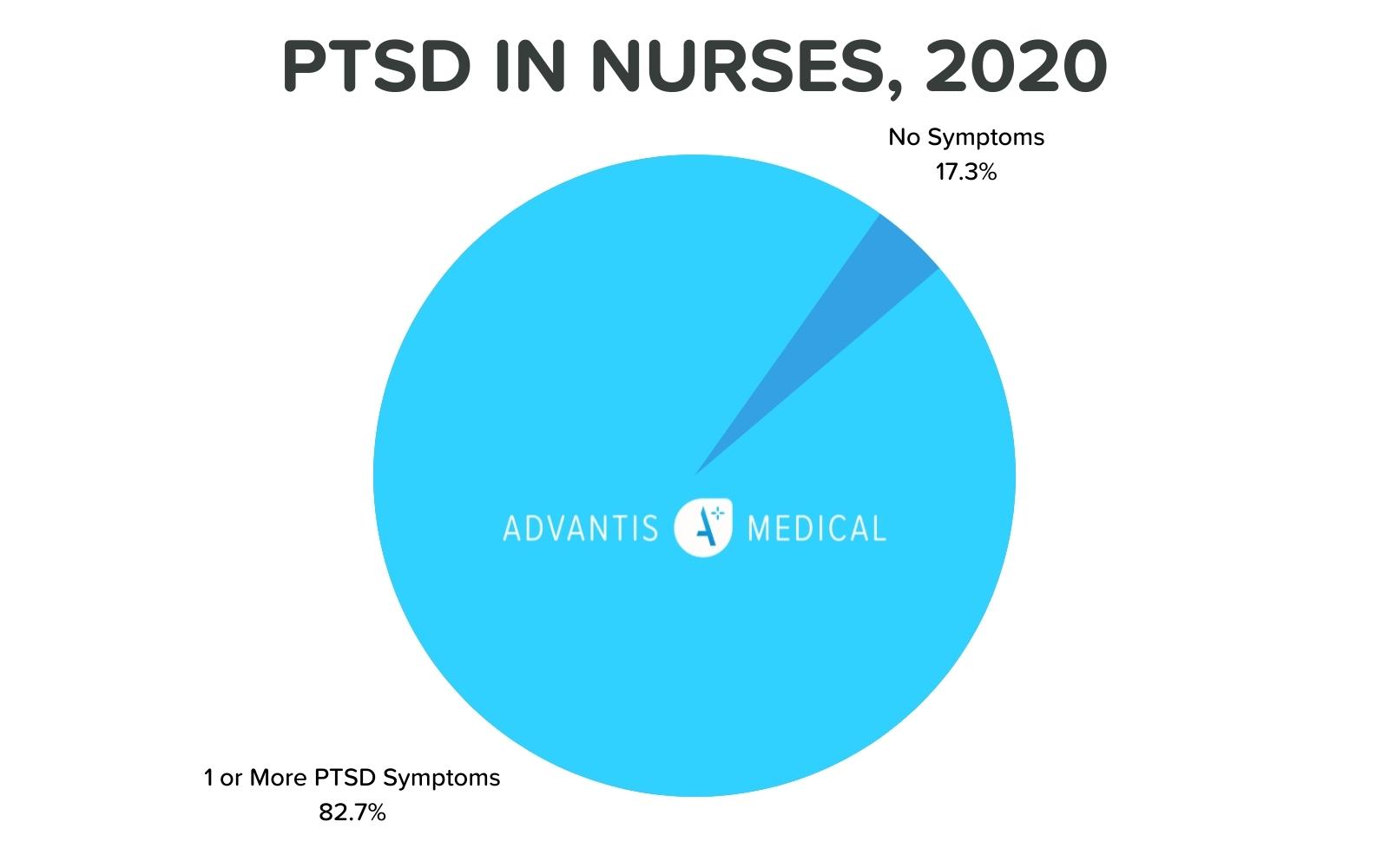
Another study in 2020 in the Journal of Clinical Nursing found that nearly 96% of nurses report at least one symptom of PTSD, and 21% meet the qualifying criteria to be clinically diagnosed. This high level of prevalence of PTSD within the nursing profession has severe implications for the sustainability of the trade.
How To Combat PTSD
To combat PTSD in nurses and health care workers, workplaces in the health care field need to provide their employees with adequate support. Workers and supervisors alike need to be supportive and compassionate towards colleagues dealing with PTSD. Those experiencing PTSD need to be allowed to discuss their feelings and be heard by their peers.
In addition to creating a PTSD nursing care plan and supportive work atmosphere for those dealing with mental illnesses, healthcare workplaces should offer debriefing or nursing interventions for PTSD sessions following traumatic events for all involved.
Nurse managers should also help connect nurses experiencing PTSD to a clinician that is trained in trauma therapy. This will allow nurses to get the expert help they need to heal and return to everyday life.
These simple changes will make a massive difference in the sustainability and longevity of nursing careers. Providing support will encourage many nurses to remain in the nursing profession. This will prevent shortages of health care workers when they are needed most.
Advantis Medical Cares
Advantis Medical is committed to connecting nurses and healthcare workers to jobs with workplaces that will value their employees’ hard work, support them, and connect them to the proper help when it is needed. In the intense world of nursing, being in a supportive and caring workplace will make all the difference in the longevity of your nursing career.
To learn more about Advantis Medical, travel nursing agency, and the services, visit our website.









